Business Name: BeeHive Homes of Granbury
Address: 1900 Acton Hwy, Granbury, TX 76049
Phone: (817) 221-8990
BeeHive Homes of Granbury
BeeHive Homes of Granbury assisted living facility is the perfect transition from an independent living facility or environment. Our elder care in Granbury, TX is designed to be smaller to create a more intimate atmosphere and to provide a family feel while our residents experience exceptional quality care. BeeHive Homes offers 24-hour caregiver support, private bedrooms and baths, medication monitoring, fantastic home-cooked dietitian-approved meals, housekeeping and laundry services. We also encourage participation in social activities, daily physical and mental exercise opportunities. We invite you to come and visit our assisted living home and feel what truly makes us the next best place to home.
1900 Acton Hwy, Granbury, TX 76049
Business Hours
Monday thru Sunday: 9:00am to 5:00pm
Facebook: https://www.facebook.com/BeeHiveHomesGranbury
YouTube: https://www.youtube.com/@WelcomeHomeBeeHiveHomes
Families generally reach assisted living at a point of stress, not leisure. A parent has fallen twice in three months. Medications have become confusing or skipped. A spouse with early dementia has begun roaming in the evening. Your house that as soon as represented stability now feels dangerous, and adult kids are pulled in between work, caregiving, and their own families.
When you start visiting senior care options, the variety is excessive. Big campuses with theaters and restaurants, little board and care homes tucked into residential areas, specialized memory care systems, brief stay respite care programs. Sales brochures guarantee security, dignity, self-reliance. What lots of households actually crave is something much simpler: a place where their loved one will be known, genuinely watched over, and not lost in a crowd.
Over the past twenty years working in elderly care, I have actually seen that little assisted living homes typically deliver that feeling of security and individual connection more regularly than very large neighborhoods. They are not the best answer for every scenario, and they bring their own restrictions, yet for lots of older adults they use a balance that feels closer to "home" than "center."
This is an effort to unload why.
What "small assisted living" normally means
The label "assisted living" covers a broad spectrum. At one end, there are resort design communities with numerous apartment or condos, numerous dining locations, and a calendar that looks like a cruise liner schedule. At the other, there are six to twelve bed homes on peaceful streets, typically converted single family homes licensed to provide senior care.
When I talk about little assisted living homes, I suggest those residential scale settings with a limited variety of homeowners, typically:
- Licensed for roughly 4 to 16 residents Staffed by a handful of caretakers per shift Located in routine neighborhoods Run by an owner or director who is on site frequently
Terminology varies by state. You will hear "board and care," "RCFE," "residential care home," or "personal care home." Laws differ, however the fundamental design is similar: assisted living and often memory care delivered in a home sized environment.
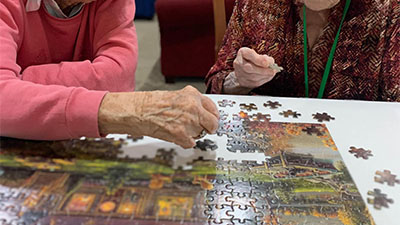
For households utilized to thinking in regards to "nursing homes," this can feel unknown. Yet for lots of older grownups who do not need complete skilled nursing, these environments fit both their care needs and their emotional needs remarkably well.
Why smaller frequently feels safer
When people say a location "feels safe," they are hardly ever referring just to grab bars and smoke alarm. They are normally describing a mix of visibility, predictability, and human attention. In a little home, a number of practical factors come together to develop that impression.
First, the scale itself restricts how much can be missed out on. In a 10 bed home, a caregiver walking from the cooking area to the living room passes most bed room doors. If a resident is trying to stand from a reclining chair unassisted, someone is most likely to observe. Casual supervision is built into the geography.
Second, staff know what "typical" appears like for each resident, typically in surprising detail. When you take care of a dozen people day after day, you learn who typically eats the entire bowl of oatmeal and who just selects at toast, whose gait is always a bit unstable and who unexpectedly seems slower this week. That baseline knowledge is critical for early detection of problems.
I keep in mind one resident, Mr. K, who resided in a 12 bed home where I consulted. He was fairly independent, still walked the yard course every morning. One day a caregiver mentioned silently, "He burnt out midway today and sat down on the bench. That is not like him." They examined his oxygen saturation, which was lower than usual, and called his medical care office. Within 24 hr he was diagnosed with a moderate pneumonia and began on treatment. In a larger setting, a single shorter walk may not have actually signed up the very same way.
Third, smaller sized homes tend to have fewer layers between decision makers and daily care. If a caregiver is fretted about a new contusion or a modification in cravings, the owner or administrator is frequently in the structure or a fast call away. There is less bureaucracy to press through before acting. Families notice that responsiveness, and it feels safe.
From an environmental viewpoint, smaller homes also typically involve:
- Shorter distances between rooms Fewer elevators and long corridors Quieter, less disorderly common areas Direct views between staff and residents
That makes a distinction for fall threat, nighttime roaming, and basic stress and anxiety. For someone with movement problems, the possibility of navigating a long corridor to reach the dining room twice a day can produce fear. Strolling twenty feet to a small dining area feels more workable, which self-confidence itself decreases risk.
The emotional side of safety
Physical safety is only part of the equation. Psychological safety matters simply as much in elderly care, specifically for those with cognitive changes.
In lots of large assisted living communities, personnel are kind and well trained, but the roster turnover and large variety of residents make deep familiarity difficult. Residents might recognize faces, however not constantly feel known. For somebody who has actually already lost parts of their memory or physical independence, that can seem like being adrift.
In small homes, relationship tends to become the organizing principle. A resident is not "in home 310." She is "Mrs. Harris, who likes chamomile tea at 8 pm and wants the paper folded before breakfast." That knowledge is not tucked away in a care plan binder. It resides in the everyday routines of the staff.
I have sat at long dining tables in these homes and seen subtle psychological care in action: a caretaker seeing that Mr. Lopez is gazing out the window a bit longer than normal and bring up a chair to ask about his favorite fishing spot, another gently rerouting a confused resident by handing them a basket of napkins to fold during an uneasy spell. These are small moments, yet for households they address one of the most fundamental fear: "Will somebody notification when my mom is struggling, even if she can not ask for aid clearly?"
That is especially vital in memory care. Residents with dementia frequently can not promote on their own, may misinterpret environments, and can escalate into stress and anxiety or agitation quickly. A little setting decreases the quantity of sensory input they need to process and permits staff to react early to subtle cues.
How care is personalized in smaller sized homes
Personalization is a trendy term, but in elderly care it has a concrete significance: how particularly does the daily regular fit the person, rather than requiring the person to fit the routine.
Large assisted living and memory care neighborhoods do strive on this. They develop personalized care strategies, ask about biography, and deal varied activities. Yet logistical realities press toward standardization. Meals at set times, group bathing schedules, medication passes done on a rigorous route.
In a little home, there is more space to bend the structure to match individual choices. That can look like:
A resident who always slept in up until 10 am being enabled to keep that routine, rather than being pulled into a 7:30 breakfast. A retired night nurse who remains more comfy keeping up later on with personnel working quietly in the cooking area close by. A devout resident having space and personal privacy set aside for day-to-day prayer at a particular hour, with personnel adjusting shower times around it.
For those with dementia, personalization can mean building the day around maintained capabilities instead of losses. I recall a lady who had been a teacher for 35 years, now in moderate stage Alzheimer's illness. She was quickly distressed in noisy groups however ended up being calmer when given tasks that looked like classroom preparation: arranging colored pencils, organizing paper stacks, "evaluating" kids's books. In a small memory care home, personnel wove that into her day naturally. In a bigger building, where activity calendars were focused on big group occasions, it had actually been harder to sustain that level of tailored engagement.
Assisted living staff in small homes also tend to know household characteristics deeply. They understand which kid is practical and wants difficult data on high blood pressure readings, and which daughter calls every night primarily requiring reassurance. That understanding lets them communicate in manner ins which pacify conflict instead of irritate it.

Staffing realities: ratios, continuity, and burnout
Families frequently ask, "What is your personnel to resident ratio?" It is a sensible question, yet it only tells part of the story.
Small assisted living homes often report ratios that look favorable on paper. For instance, 2 caretakers for 10 citizens during the day, and one awake overnight, often with a reside in employee on the properties. Larger communities may have more complex staffing structures, with different med techs, caregivers, and nurses rotating throughout wings.
The benefit in little homes is less about the raw ratio and more about connection. The exact same two or three caregivers tend to cover a lot of weekday shifts, another small group covers weekends. Homeowners and personnel recognize each other quickly. Caretakers discover which locals can wait five minutes for a bathroom call and which can not, who is safe to stroll behind unaided and who need to be side by side, who will attempt to get up from bed without calling at 3 am if they consumed tea too late.
Continuity likewise decreases mistakes. A familiar caregiver is more likely to capture that a medication blister pack looks different this month and concern it. They are more likely to notice weight modifications when assisting a resident dress. In memory care, they rapidly see when a new habits becomes part of a pattern or a separated incident.

The challenge, obviously, is that small homes often run lean. If one caretaker calls out sick at short notice, there is less backup. Owners who run these homes well build swimming pools of on call personnel, step in themselves, and maintain cross training. Households examining a home should not just ask about typical staffing, however likewise how the home manages spaces, getaways, and emergencies.
Burnout is another quiet factor. In a big structure, personnel may be stretched thin across numerous locals, yet the work is rather dispersed. In a little setting, if care requirements increase suddenly for 2 or three individuals simultaneously, the problem can land heavily on a small staff group. Good operators react by including additional hours, contacting company aid temporarily, or bringing hospice partners into the discussion. Poor operators merely push personnel harder and hope no one falls.
When small homes listen to staffing health, the result is a level of caregiving stability that homeowners and households feel immediately. I have actually seen caregivers remain with the very same 8 bed home for a decade, shepherding residents from their very first day of relocation in through the last days of hospice. That sort of continuity is extremely rare in institutional settings.
Memory care in a small setting: guarantee and limits
Dedicated memory care systems inside big neighborhoods can provide protected borders, specialized activity programs, and nursing oversight. They are vital resources for lots of families. Yet they can likewise feel overstimulating for homeowners in mid or later phases of dementia: Televisions in typical areas, overhead announcements, a continuous parade of staff.
Small memory care homes that take only homeowners with cognitive disability approach safety differently. Rather than locking down a big courtyard, they may fence a manageable garden where every corner is visible from the back porch. Rather of a huge group activity room, they count on the living-room, dining table, and yard as natural event spaces.
The advantages are simple. A resident who begins to speed is never far from a familiar caregiver. Noise levels are simpler to manage. Triggers for agitation, like crowded hallways or a lot of unfamiliar faces, are reduced.
However, small memory care homes likewise have difficult limits. They rarely have certified nurses on site 24 hours a day. If a resident establishes severe behavioral signs requiring regular medication changes, or intricate medical problems like innovative diabetes management, they may be better served in a larger community with more powerful scientific facilities or in a nursing facility.
Families sometimes feel blindsided when a little home says, "We can no longer safely satisfy your loved one's requirements." From the operator's perspective, this is often an ethical choice rather than a benefit. A 10 bed home without night nursing can not securely handle a resident who begins to fall multiple times a week in spite of interventions, or who becomes physically aggressive, placing others at risk.
Understanding this from the beginning assists. When you tour, ask straight: "What type of modifications would make you say that my parent needs a higher level of care?" A transparent response is an excellent sign.
Respite care: attempting small assisted living on for size
For households who are uncertain whether their loved one will endure a relocation, respite care can supply a low commitment trial. Numerous small assisted living and memory care homes provide short stays, frequently from one week to a few months, where a senior lives in the home momentarily while receiving the same level of support as long term residents.
Respite stays serve a number of functions. They provide the older grownup a possibility to experience the environment without the pressure of a permanent choice. They give the household a much needed break from round the clock caregiving. And they let everybody assess fit: Is mom more unwinded in this smaller setting, or does she seem tired? Is dad less nervous in the evening when staff neighbor, or does he bristle at any loss of control?
I worked with a household caring for an 84 year old father with moderate dementia and significant nighttime roaming. The child was persuaded he would decline any relocation, yet she was sleeping with one eye open every night, terrified of him leaving your house. They arranged a 3 week respite remain in a six bed memory care home under the pretext of "helping Dad recover after a healthcare facility visit." To the daughter's astonishment, he settled quickly and began signing up with small group tunes in the living-room each afternoon. By the 2nd week, she told me, "He in fact seems calmer there than in the house." That respite stay eventually became a permanent move, however since it began as a short-lived step, everybody felt less trapped by the decision.
Respite care is also a chance to test how the home communicates. During the stay, you need to get updates about sleep, appetite, mood, and any events. Take note not just to what is reported, however to the tone. Are personnel just documenting events, or do they offer thoughtful observations and adjustments?
When a bigger neighborhood might be better
Small assisted living homes are not a universal service. There are clear situations where a larger neighborhood or higher level of care is more appropriate.
Residents with complicated medical needs that verge on experienced nursing typically need the on website existence of certified nurses, rehabilitation therapists, and frequent doctor oversight. For instance, someone with stage IV heart disease on multiple titrated medications, or an insulin dependent diabetic with highly labile blood sugar level, might surpass what a little residential home can safely manage.
Some older adults genuinely love more stimulation than a small home can offer. Extroverted citizens who take pleasure in constant activity choices, structured classes, and a wide range of peers may find a little group limiting. I took care of a retired music professor who lasted exactly three weeks in a cozy eight bed home before stating, quite fairly, that he missed out on the energy of the larger continuing care community he had previously visited. He relocated to the bigger campus, signed up with three clubs within a month, and was clearly happier.
Couples with mismatched needs often find better alternatives in bigger settings too. If the wife requires memory care and the other half is still reasonably independent, a community with both assisted living and independent living beehivehomes.com memory care on one campus can minimize separation. Some little homes can take the partner with greater requirements and enable the healthier partner to visit daily, yet that plan is not always sustainable.
Cost and location likewise matter. Little homes in particular regions are scarce or priced higher than mid market assisted living neighborhoods. Families in some cases need to consider proximity to their own homes, particularly if they prepare to visit a number of times a week.
The secret is to view little homes as one tool in the senior care tool kit, not a universal response. The best fit depends upon care requirements, personality, family involvement, and monetary reality.
What to search for when exploring a small assisted living home
A polished website or kind marketing director can not replacement for what you observe in person. When you tour, your senses are your finest guides. One focused list can help you arrange impressions without lowering the experience to numbers alone.
Consider paying unique attention to these points during your visit:
- Staff existence: Are caregivers noticeable, engaged with locals, and calm, or are they mostly in the workplace or kitchen? Resident mood: Do residents look typically relaxed, groomed, and appropriately dressed, or do numerous seem distressed or unattended? Cleanliness and smells: Does the home odor like a lived in home, or are there persistent odors of urine, severe chemicals, or heavy air freshener covering something else? Communication design: Do staff address citizens by name, make eye contact, and discuss what they are doing, or do they discuss residents as if they are not present? Flexibility: When you ask about personalized regimens, do you hear particular examples of how they adapt, or only rigid schedules that everyone should follow?
During a good tour, you should feel able to ask direct questions about falls, hospitalizations, and staff turnover. Transparent homes do not pretend bad things never happen. Instead, they describe what they found out and how they adjusted.
Also observe how they talk about residents with amnesia. Language matters. Staff who speak respectfully, avoid labels like "wanderer" or "challenging," and concentrate on staying strengths reflect a much deeper culture of dignity.
Key questions to ask the administrator or owner
A list of targeted questions can reveal more than an inch thick packet of printed policies. When you meet the administrator or owner of a little assisted living or memory care home, you may utilize questions such as:
- "Can you explain a resident whose needs ended up being undue for you to handle, and how you dealt with that transition with the family?" "When a caretaker calls out at the last minute, what does your backup strategy really look like on a Saturday night?" "How do you collaborate with hospice or home health if my parent ultimately requires those services here?" "Tell me about a time something failed - a fall, a medication error - and what altered afterward." "If my parent becomes more baffled or agitated in the evening, what specific methods do your personnel usage before turning to medication?"
Notice how they react. Honest operators may confess past mistakes and explain practical enhancements. Avoid places that immediately resort to unclear assurances or end up being protective when pressed.
Balancing head and heart in the last choice
Choosing an assisted living, memory care, or respite care setting for somebody you like is one of the more mentally filled choices most households will ever make. It sits at the intersection of safety, autonomy, finances, and long held household promises.
Small assisted living homes typically feel much safer and more personal due to the fact that they compress that choice into a human scale environment. Regimens are visible. Personnel are not distant uniforms but people you welcome by name. Your mother's preferred chair can fit in the living room. The cook knows which dessert your father must avoid due to the fact that of his blood glucose, and which he will accept alternative fruit for without feeling punished.
Those qualities do not appear by mishap. They grow from thoughtful staffing, attentive management, and an understanding that elderly care is as much relational as it is clinical. When succeeded, little homes can provide an environment where older grownups, even with substantial needs, still experience days that make sense, feel seen, and keep a sense of belonging.
The work for families is to look beyond layout and facilities lists, to evaluate those relational qualities with mindful questions, honest observation, and, when possible, short respite stays. Numbers such as personnel ratios and regular monthly charges are essential, yet the quieter indications - a hand on a resident's shoulder at the ideal moment, a team member who remembers your father's war stories from last visit - are often the ones that tell you whether this specific home will truly feel both much safer and more personal.
BeeHive Homes of Granbury provides assisted living care
BeeHive Homes of Granbury provides memory care services
BeeHive Homes of Granbury provides respite care services
BeeHive Homes of Granbury supports assistance with bathing and grooming
BeeHive Homes of Granbury offers private bedrooms with private bathrooms
BeeHive Homes of Granbury provides medication monitoring and documentation
BeeHive Homes of Granbury serves dietitian-approved meals
BeeHive Homes of Granbury provides housekeeping services
BeeHive Homes of Granbury provides laundry services
BeeHive Homes of Granbury offers community dining and social engagement activities
BeeHive Homes of Granbury features life enrichment activities
BeeHive Homes of Granbury supports personal care assistance during meals and daily routines
BeeHive Homes of Granbury promotes frequent physical and mental exercise opportunities
BeeHive Homes of Granbury provides a home-like residential environment
BeeHive Homes of Granbury creates customized care plans as residents’ needs change
BeeHive Homes of Granbury assesses individual resident care needs
BeeHive Homes of Granbury accepts private pay and long-term care insurance
BeeHive Homes of Granbury assists qualified veterans with Aid and Attendance benefits
BeeHive Homes of Granbury encourages meaningful resident-to-staff relationships
BeeHive Homes of Granbury delivers compassionate, attentive senior care focused on dignity and comfort
BeeHive Homes of Granbury has a phone number of (817) 221-8990
BeeHive Homes of Granbury has an address of 1900 Acton Hwy, Granbury, TX 76049
BeeHive Homes of Granbury has a website https://beehivehomes.com/locations/granbury/
BeeHive Homes of Granbury has Google Maps listing https://maps.app.goo.gl/xVVgS7RdaV57HSLu9
BeeHive Homes of Granbury has Facebook page https://www.facebook.com/BeeHiveHomesGranbury
BeeHive Homes of Granbury has an YouTube page https://www.youtube.com/@WelcomeHomeBeeHiveHomes
BeeHive Homes of Granbury won Top Assisted Living Homes 2025
BeeHive Homes of Granbury earned Best Customer Service Award 2024
BeeHive Homes of Granbury placed 1st for Senior Living Communities 2025
People Also Ask about BeeHive Homes of Granbury
What is BeeHive Homes of Granbury Living monthly room rate?
The rate depends on the level of care that is needed. We do an initial evaluation for each potential resident to determine the level of care needed. The monthly rate is based on this evaluation. There are no hidden costs or fees
Can residents stay in BeeHive Homes until the end of their life?
Usually yes. There are exceptions, such as when there are safety issues with the resident, or they need 24 hour skilled nursing services
Do we have a nurse on staff?
No, but each BeeHive Home has a consulting Nurse available 24 – 7. if nursing services are needed, a doctor can order home health to come into the home
What are BeeHive Homes’ visiting hours?
Visiting hours are adjusted to accommodate the families and the resident’s needs… just not too early or too late
Do we have couple’s rooms available?
Yes, each home has rooms designed to accommodate couples. Please ask about the availability of these rooms
Where is BeeHive Homes of Granbury located?
BeeHive Homes of Granbury is conveniently located at 1900 Acton Hwy, Granbury, TX 76049. You can easily find directions on Google Maps or call at (817) 221-8990 Monday through Sunday 9:00am to 5:00pm
How can I contact BeeHive Homes of Granbury?
You can contact BeeHive Homes of Granbury by phone at: (817) 221-8990, visit their website at https://beehivehomes.com/locations/granbury/, or connect on social media via Facebook or YouTube
Eighteen Ninety Grille and Lounge offers classic comfort food in a setting appropriate for assisted living, memory care, senior care, elderly care, and respite care dining visits.